Heart Attack – Signs & Symptoms
How do you survive a heart attack? Fast action is your best weapon against a heart attack. Why? Because medical treatments can stop a heart attack in its tracks. They can prevent or limit damage to the heart–but they need to be given immediately after symptoms begin. The sooner they are started, the more good they will do – and the greater the chances are for survival and a full recovery. To be most effective, they need to be given ideally within 1 hour of the start of heart attack symptoms.
- Uncertainty is Normal
- Delay Can Be Deadly
- Call 9-1-1
- Emergency Medical Personnel
- Plan Ahead
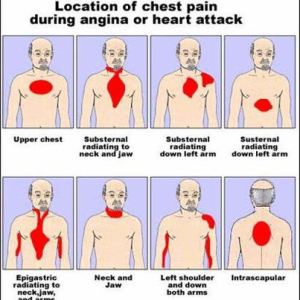
Discomfort or a heavy feeling in the chest can signal a heart attack.
Chest pain is the most commonly reported heart attack symptom. But the pain may not feel severe or “stabbing.” It may feel more like a discomfort. Chest discomfort may be accompanied by or follow shortness of breath. Or discomfort or pain may be felt in other areas of the upper body, such as one or both arms, the back, neck, jaw, or stomach.
Also, other symptoms that can occur include breaking out in a “cold sweat,” nausea, or light-headedness.
Women frequently experience heart attacks.
Heart disease is the number one killer of American women, and nearly half of all heart attack deaths each year happen to women. Furthermore, women are less likely to survive a heart attack than are men.
African-American women have higher risk of dying of heart attacks than white
African-American women’s death rates from heart attacks are a third higher than the rates for white women. In general, women and minorities delay longer before calling for help. African-American women also are at greater risk for hypertension and diabetes, which are both risk factors for heart disease. More on Women and Heart Attacks.
Some people who are experiencing the symptoms of a heart attack may wait hours or even days before seeking needed medical care.
Many people do not recognize their symptoms as life-threatening. That’s why it is important to know the warning signs and take action quickly.
Being treated within about an hour of the first symptoms can make a significant difference.
Heart attack deaths and heart damage can often be avoided when treatment begins within an hour of when the symptoms started. Most studies show a large reduction in death rates and in heart damage in patients treated within 1 hour of the start of symptoms.
Many heart attack victims say their heart attack wasn’t what they’d expected.
Most people expect a heart attack to be a sudden intense pain, but often heart attacks start slowly as a mild pain. Patients whose experience did not match their expectations delayed longer before seeking treatment. And delay costs lives.
A family member, such as a spouse, can persuade a loved one having a heart attack to seek help immediately.
True but studies tell us that family members should expect lack of awareness or denial of the seriousness of the symptoms, and resistance to calling for help. Many heart attack sufferers will reject calling 9-1-1, thus delaying the arrival of help. That’s why it’s best to enlist family, friends, and coworkers now. Discuss the symptoms. Talk to your doctors about risk for a heart attack. Make a survival plan, before you need one. Whenever a heart attack is suspected, everyone should know to call 9-1-1 immediately–wait no longer than 5 minutes, if symptoms persist. Don’t wait for the person having symptoms to agree. Take charge to make sure the person gets checked out sooner rather than later.
Calling 9-1-1 for chest pain alone would probably turn out to be a waste of the emergency medical personnel’s time.
It’s better to be safe than sorry, and sometimes chest pain—even mild chest pain—is the only indicator of a heart attack beginning. Emergency medical personnel, or mobile EMS teams, can diagnose a heart attack and begin treatments on the spot. They can even revive a heart that has stopped or is beating erratically. Call right away—do not wait longer than 5 minutes from when symptoms start. It’s okay to be wrong. Emergency medical personnel want you to call to get a heart attack checked out. And even if the call turns out to be a false alarm, running the risk of feeling a little embarrassed is better than running the risk of dying or having a permanently damaged heart.
Most heart attacks occur in people over 65.
However, 45 percent, or nearly half, of all heart attacks occur in people under age 65. Five percent occur in people under age 40.
The major issue in delay is how long it takes for emergency medical personnel to find the address and deliver the patient to the hospital.
The most significant portion of delay time is due to patient delay, the time it takes for an individual to decide to ask for help. Sometimes a patient does not want to believe anything bad is happening and dismisses the seriousness of the symptoms.
Sometimes people do not know the symptoms of heart attack.
Frequently Asked Questions About Heart Attack:
Heart Attack Warning Signs—
Q: How would I know if I were having a heart attack?
Often, it is not easy to tell. But there are symptoms people may have. These are:
- an uncomfortable pressure,
- squeezing, fullness, or
- pain in the center of the chest that lasts more than a few minutes, or goes away and comes back;
- discomfort in other areas of the upper body, which may be felt in one or both arms, the back, neck, jaw, or stomach;
- shortness of breath, which often occurs with or before chest discomfort;
- and other symptoms such as breaking out in a cold sweat, nausea, or light-headedness. When in doubt, check it out! Call 9-1-1. Don’t wait more than a few minutes– 5 at most. Call right away!
Q: What is angina and how is it different from a heart attack?
An episode of angina is NOT a heart attack. However, people with angina report having a hard time telling the difference between angina symptoms and heart attack symptoms. Angina is a recurring pain or discomfort in the chest that happens when some part of the heart does not receive enough blood temporarily. A person may notice it during exertion (such as in climbing stairs). It is usually relieved within a few minutes by resting or by taking prescribed angina medicine. People who have been diagnosed with angina have a greater risk of a heart attack than do other people.
.
Pre-hospital Delay Time—
.
Q: I’d rather wait until I’m sure something’s really wrong. What’s the rush anyway?
Medical treatments work best when given within the first hour after a heart attack starts. The first hour also is the most risky time during a heart attack–it’s when your heart might stop suddenly. Responding fast to your symptoms really increases your chance of surviving.
.
Q: So how quickly should I act?
If you have any heart attack symptoms, call 9-1-1 immediately. Don’t wait for more than a few minutes–5 at most–to call 9-1-1.
.
Q: Why should I bother? If I’m going to die, there’s not much I can do about it anyway, is there?
That’s not true. There is something that can be done about a heart attack. Doctors have medical procedures that can stop or reverse a heart attack, if given quickly. These drugs can limit the damage to the heart muscle by removing the blockage and restoring blood flow. Less heart damage means a better quality of life after a heart attack.
Given that these new therapies are available, it’s very sad to know that so many people cannot receive these treatments because they delay too long before seeking care. The greatest benefits of these therapies are gained when patients come in early (preferably within the first hour of the start of their symptoms).
The Role of Emergency Medical Personnel—
Q: Emergency medical personnel cause such a commotion. Can’t I just have my wife/husband/friend/coworker take me to the hospital?
Emergency medical personnel—also called EMS, for emergency medical services—bring medical care to you. For example, they bring oxygen and medications. And they can actually restart someone’s heart if it stops after they arrive. Your wife/husband/friend/coworker can’t do that, or help you at all if they are driving. In the ambulance, there are enough people to give you the help you need and get you to the hospital right away.
Steps to Survival—
Q: I’m not sure I can remember all this. What can I do to make it easier for me?
You can make a plan and discuss it in advance with your family, your friends, your coworkers and, of course, your doctor. Then you can rehearse this plan, just like a fire drill. Keep it simple. Know the warning signs. Keep information–such as what medications you’re taking–in one place. If you have any symptoms of a heart attack for a few minutes (no more than 5), call the EMS by dialing 9-1-1 right away.
.
Q: I carry nitroglycerin pills all the time for my heart condition. If I have heart attack symptoms, shouldn’t I try them first?
Yes, if your doctor has prescribed nitroglycerin pills, you should follow your doctor’s orders. If you are not sure about how to take your nitroglycerin when you get chest pain, check with your doctor.
.
Q: What about taking an aspirin like we see on television?
You should not delay calling 9-1-1 to take an aspirin. Studies have shown that people sometimes delay seeking help if they take an aspirin (or other medicine). Emergency department personnel will give people experiencing a heart attack an aspirin as soon as they arrive. So, the best thing to do is to call 9-1-1 immediately and let the professionals give the aspirin.
What Are the Signs and Symptoms of Angina?
Angina
Pain and discomfort are the main symptoms of angina. These symptoms include:
- Are often described as pressure, squeezing, burning, or tightness in the chest
- Usually start in the chest behind the breastbone
- May also occur in the arms, shoulders, neck, jaw, throat, or back
- May feel like indigestion
Some people say that angina discomfort is hard to describe or that they can’t tell exactly where the pain is coming from. Symptoms such as nausea, fatigue, shortness of breath, sweating, light-headedness, or weakness may also occur.
Symptoms vary based on the type of angina.
Stable Angina
- The pain or discomfort:
- Occurs when the heart must work harder, usually during physical exertion
- Is expected, and episodes of pain tend to be alike
- Usually lasts a short time (5 minutes or less)
- Is relieved by rest or angina medicine
- May feel like gas or indigestion
- May feel like chest pain that spreads to the arms, back, or other areas
Unstable Angina
The pain or discomfort:
- Often occurs at rest, while sleeping at night, or with little physical exertion
- Is unexpected
- Is more severe and lasts longer (as long as 30 minutes) than episodes of stable angina
- Is usually not relieved with rest or angina medicine
- May get continuously worse
- May signal that a heart attack will happen soon
Variant Angina
The pain or discomfort:
- Usually occurs at rest and during the night or early morning hours
- Tends to be severe
- Is relieved by angina medicine
Chest pain that lasts longer than a few minutes and is not relieved by rest or angina medicine may mean you are having—or are about to have—a heart attack. Call 9–1–1 right away.
What Are the Signs and Symptoms of Atherosclerosis?
Atherosclerosis
Atherosclerosis usually does not cause symptoms until it:
- Severely narrows an artery
- Totally blocks an artery
Symptoms you may have depend on which arteries are severely narrowed or blocked.
If the arteries that feed your heart (coronary arteries) are affected, you have symptoms of coronary artery disease.
- If the arteries that feed your brain are affected, you have symptoms of a stroke or a transient ischemic attack (TIA) or “mini stroke.”
- If the arteries that feed your legs, pelvis, or arms are affected, you have symptoms of peripheral arterial disease.
- If the arteries that feed your kidneys are affected, you have symptoms of renovascular hypertension.
What Are the Signs and Symptoms of Coronary Artery Disease?
Coronary Artery Disease
The most common symptoms of coronary artery disease (CAD) are:
- Chest pain or chest discomfort (angina) or pain in one or both arms or in the left shoulder, neck, jaw, or back
- Shortness of breath
The severity of symptoms varies widely. Symptoms may become more severe as coronary arteries become narrower due to the buildup of plaque (atherosclerosis).
.
In some people, the first sign of CAD is a heart attack. A heart attack happens when plaque in a coronary artery breaks apart, causing a blood clot to form and block the artery.
.
What Are the Signs and Symptoms of a Heart Attack?
Not all heart attacks begin with a sudden, crushing pain that is often shown on TV or in the movies. The warning signs and symptoms of a heart attack aren’t the same for everyone. Many heart attacks start slowly as mild pain or discomfort. Some people don’t have symptoms at all (this is called a silent heart attack).
The most common symptom of heart attack is chest pain or discomfort. Most heart attacks involve discomfort in the center of the chest that lasts for more than a few minutes or goes away and comes back. The discomfort can feel like uncomfortable pressure, squeezing, fullness, or pain. It can be mild or severe. Heart attack pain can sometimes feel like indigestion or heartburn.
.
The symptoms of angina can be similar to the symptoms of a heart attack. Angina is pain in the chest that occurs in people with coronary artery disease, usually when they’re active. Angina pain usually lasts for only a few minutes and goes away with rest. Angina that doesn’t go away or that changes from its usual pattern (occurs more frequently or occurs at rest) can be a sign of the beginning of a heart attack and should be checked by a doctor right away.
- Other Common Signs and Symptoms
Other common signs and symptoms that a person can have during a heart attack include:
- Upper body discomfort in one or both arms, the back, neck, jaw, or stomach. Shortness of breath may often occur with or before chest discomfort
- Nausea (feeling sick to your stomach), vomiting, lightheadedness or fainting, or breaking out in a cold sweat
Not everyone having a heart attack experiences the typical symptoms. If you’ve already had a heart attack, your symptoms may not be the same for another one. The more signs and symptoms you have, the more likely it is that you’re having a heart attack.
Act Fast!
Sometimes the signs and symptoms of a heart attack happen suddenly, but they can also develop slowly, over hours, days, and even weeks before a heart attack occurs.
Know the warning signs of a heart attack so you can act fast to get treatment for yourself or someone else. The sooner you get emergency help, the less damage there will be to your heart.
Call 9–1–1 for help within 5 minutes if you think you may be having a heart attack or if your chest pain doesn’t go away as it usually does when you take prescribed medicine.
Don’t drive yourself or anyone else to the hospital. Call an ambulance so that medical personnel can begin life-saving treatment on the way to the emergency room.
What Are the Signs and Symptoms of Heart Failure?
The most common signs and symptoms are:
- Shortness of breath or difficulty breathing
- Swelling in the ankles, feet, legs, and sometimes the abdomen
- Shortness of breath and feeling tired are caused by the buildup of fluid in the lungs and around the lungs (pleural effusions). When symptoms start, you may feel tired and short of breath after routine physical exertion. Climbing two flights of stairs makes you feel winded. As heart failure progresses, the symptoms get worse. You may begin to feel tired and short of breath after simple activities, like getting dressed or walking across the room. Some people have shortness of breath when lying flat.
- Fluid buildup in the lungs can also cause a cough. The cough is worse at night and when you are lying down. Excessive fluid in the lungs can cause a life-threatening condition called acute pulmonary edema. This condition requires emergency treatment.
The swelling is from the buildup of fluid in your body (edema). Other signs of fluid buildup are:
- Weight gain
- Frequent urination
Limitation on Physical Activity
Doctors also classify your symptoms based on how much they limit your daily activity. By class of symptom, your doctor means:
- Class 1: No limits—ordinary physical activity does not cause undue tiredness or shortness of breath.
- Class 2: Slight or mild limits—comfortable at rest, but ordinary physical activity results in tiredness or shortness of breath.
- Class 3: Marked or noticeable limits—comfortable at rest, but less than ordinary physical activity causes tiredness or shortness of breath.
- Class 4: Severe limits—unable to carry on any physical activity without discomfort. Symptoms are also present at rest. If any physical activity is undertaken, discomfort increases.
What Are the Signs and Symptoms of Chronic Heart Failure and Acute Heart Failure?
Chronic heart failure
Signs and symptoms of chronic heart failure can include:
- Fatigue and weakness
- Shortness of breath (dyspnea) when you exert yourself or when you lie down
- Reduced ability to exercise
- Persistent cough or wheezing with white or pink blood-tinged phlegm
- Swelling (edema) in your legs, ankles and feet
- Swelling of your abdomen (ascites)
- Sudden weight gain from fluid retention
- Lack of appetite and nausea
- Difficulty concentrating or decreased alertness
- Irregular or rapid heartbeat
Acute heart failure
Signs and symptoms of acute heart failure can include:
Acute heart failure can occur when something suddenly affects your heart’s ability to function. Signs and symptoms of acute heart failure are similar to those of chronic heart failure, but are more severe and start or worsen suddenly. Signs and symptoms of acute heart failure may include:
- Sudden fluid buildup
- Rapid or irregular heartbeat with palpitations
- Sudden, severe shortness of breath and coughing up pink, foamy mucus
- Chest pain if caused by a heart attack or a bulge in an artery (aneurysm)
What Is a Heart Murmur?
Heart Murmur:
A heart murmur is an extra or unusual sound heard during your heartbeat. Murmurs range from very faint to very loud and sometimes sound like a whooshing or swishing noise. Normal heartbeat sounds—”lub-DUPP” or “lub-DUB”—are the valves closing as blood moves through the heart.
A heart murmur is not a disease; it is a sound that the doctor hears with a stethoscope. It may be normal, or it could be a sign that something may be wrong. Most heart murmurs are harmless. Some are signs of heart problems, especially if other signs or symptoms of a heart problem are present.
.
Types of Murmurs
- Innocent (harmless) murmurs
- A person with an innocent murmur has a normal heart and usually has no other signs or symptoms of a heart problem. Innocent murmurs are common in healthy children.
- Abnormal murmurs
- A person with an abnormal murmur usually has other signs or symptoms of a heart problem. Most abnormal murmurs in children are due to congenital heart defects—heart defects present at birth. In adults, abnormal murmurs are most often due to heart valve problems caused by infection, disease, or aging.
.
What Are the Signs and Symptoms of Hypotension?
Hypotension:
Orthostatic Hypotension
The symptoms of orthostatic hypotension happen within a few seconds or minutes of a person standing up after sitting or lying down. They go away if the person sits or lies down again. The signs and symptoms of orthostatic hypotensioninclude:
- Dizziness or feeling lightheaded
- Blurry vision
- Confusion
- Feeling faint or weak
- Fainting
Neurally Mediated Hypotension
The symptoms of neurally mediated hypotension (NMH) happen after a person has been standing for a long time or in response to an unpleasant, upsetting, or frightening situation. Like orthostatic hypotension, the drop in blood pressure with NMH is temporary and usually goes away after the person sits down. The signs and symptoms of neurally mediated hypotension NMH are similar to those of orthostatic hypotension.
.
Severe Hypotension Associated With Shock
In shock, not enough blood flows to the major organs, including the brain.
The early signs and symptoms of reduced blood flow to the brain include lightheadedness, sleepiness, and confusion. In the earliest stages of shock, it may be hard to detect any signs and symptoms. In older people, the first symptom may only be confusion.
As shock worsens, eventually, the person cannot sit up without passing out. If it continues, the person will lose consciousness. Shock is often fatal if not treated.
Some of the other signs and symptoms of shock vary, depending on the cause. When shock is caused by low blood volume (such as from massive bleeding) or poor pumping action by the heart (as in heart failure):
- The skin becomes cold and sweaty. It often looks blue or pale. If pressed, the color returns more slowly than normal. A bluish network of lines can be seen under the skin.
- The pulse becomes weak and rapid.
- The person begins to breathe very quickly.
When shock is caused by extreme widening or stretching of blood vessels (such as in septic shock), a person feels warm and flushed at first. Later, the skin becomes cold and clammy, and the person feels very sleepy.
What Are the Signs and Symptoms of Marfan Syndrome?
Marfan Syndrome
The signs and symptoms of Marfan syndrome vary from one person to another, even within the same family. Some people have mild signs and symptoms, while others may have severe problems and discomfort. Signs and symptoms of Marfan syndrome occur in many parts of the body, including:
- The bones and ligaments
- The heart and blood vessels
- The eyes
- The lungs
- The skin
Appearance and Body Build
Some of the major signs of Marfan syndrome are the common physical features seen in people with the condition. People with Marfan syndrome often have:
- A tall, slender body build. They may be very tall or taller than other family members who do not have the condition. However, it should be noted that short, heavy people also can have Marfan syndrome.
- Long arms, legs, fingers, and toes. A person’s arm span (the distance from the fingertips of one hand to the fingertips of the other with the arms stretched out from the sides) may be greater than his or her height.
- A long and narrow face.
- A highly arched roof of the mouth with crowded teeth.
- A receding lower jaw, causing an overbite.
- A protruding or sunken chest.
- A curved spine.
- Flat feet that are rotated inward (some people, however, have exaggerated arches).
Bones, Cartilage, and Ligaments
The bones of the limbs, hands, and feet often grow too long in people with Marfan syndrome. This typically leads to a tall, thin body with disproportionately long arms, fingers, legs, and toes. People with Marfan syndrome have loose, relaxed ligaments and are usually loose jointed.
.
Chest abnormalities may occur due to an overgrowth of the ribs. There are two types of chest abnormalities:
- Pigeon breast, also called pectus carinatum. The chest protrudes outward like a bird’s chest. This can affect heart and lung function.
- Funnel chest, also called pectus excavatum. The chest is sunken or indented, reducing the space between the breastbone and the backbone. As a result, the heart and lungs are displaced. Heart and lung function may be affected, leading to breathing and endurance problems.
Curvature of the spine may occur. It usually develops during childhood, often gets worse during the teenage growth spurt, and may require surgical treatment. The three main types of abnormal spine curvature are:
- Scoliosis—a side-to-side curvature
- Lordosis—an inward curvature of the spine in the lower back, just above the buttocks
- Kyphosis—an outward curvature of the spine in the upper back (hunchback)
Curvature of the spine can cause back pain, posture problems, and deformity. Scoliosis can sometimes reduce lung function.
Another problem that can occur is dural ectasia (ek-TA-ze-a), which is the stretching of the membrane surrounding the brain and spinal cord. Dural ectasia can wear down the bones of the spine over time. Symptoms dural ectasia may include:
- Pain in the lowest part of the back
- Pain in the abdomen
- Pain, numbness, or weakness of the legs
Dural ectasia is a hallmark of Marfan syndrome that is very rare in the general population.
.
Heart and Blood Vessels
People who have Marfan syndrome often have problems with the heart and blood vessels. The valves of the heart may not work properly and may permit some blood flow to be reversed, causing the heart to do extra work. The aorta—the large artery that carries blood away from the heart to the body—may stretch and enlarge. These problems can cause signs and symptoms, such as:
- A heart murmur. This can be the result of valves not functioning properly or other heart problems.
- Sudden chest pain. This can be a symptom of aortic dissection, a life-threatening complication that can occur due to weakened aorta walls. The pain may occur in the front or in the back, usually in the midline of the body. The location of the pain may change as the tear in the aorta grows. In some cases, a dissection does not cause dramatic pain.
- Abnormal heart rhythms called arrhythmias (a-RITH-me-as). A person with Marfan syndrome may develop an arrhythmia as a result of problems with the heart valves or due to cardiomyopathy or congestive heart failure.
- Shortness of breath and fatigue (tiredness). These can be symptoms of heart failure due to an overworked heart.
Two of the heart and blood vessel complications that can occur in people with Marfan syndrome are mitral valve prolapse (MVP) and enlargement of the aorta.
Mitral Valve Prolapse:
MVP is a problem with the heart’s mitral valve. The mitral valve controls the flow of blood through two of the chambers in the heart, the left atrium and the left ventricle. The flaps of the valve are designed to allow blood to flow in one direction—from the left atrium into the left ventricle—and to prevent blood from flowing the other way.
In MVP, the mitral valve does not work correctly. The valve flaps are large and floppy. They may overlap or not close completely. One or both flaps may flutter or swing back into the atrium.
.
The abnormal mitral valve can allow blood to flow backward through the valve in the wrong direction. This is called mitral regurgitation. When this happens, the heart has to work harder to make up for the backward flow of blood. Over time, the heart can become overworked, leading to heart failure.
MVP occurs in about 3 out of every 4 people with Marfan syndrome. It also occurs in people who do not have Marfan syndrome. In many people with MVP, little or no blood leaks back through the valve, there are no symptoms, and no treatment is needed. In some people, blood does leak back through the valve, and these people may have symptoms and require treatment.
.
Enlargement of the Aorta (Aortic Dilation)
The aorta is the large artery that carries oxygen-rich blood away from your heart out to the rest of the body. When weak connective tissue causes the walls of the aorta to weaken, the aorta widens and stretches. Most often, the enlargement begins where the aorta connects with the left ventricle of the heart, just above the aortic valve. This part of the aorta is called the aortic root.
.
Enlargement of the aorta can lead to several serious complications:
- Aortic root dilation. The aorta can widen and bulge where it attaches to the heart. This happens due to continued weakening of the wall of the aorta. Aortic root dilation may not cause any symptoms until it becomes quite large. If symptoms occur, they may include pain in the chest, upper back, neck, and jaw; coughing and hoarseness; and trouble swallowing. As part of this dilation, one section may enlarge and bulge out. This is called an aortic aneurysm (AN-u-rism). The aneurysm can rupture, causing massive internal bleeding, which is a life-threatening medical emergency.
- Aortic regurgitation. The aortic valve sits between the left ventricle and the aorta and allows blood to flow one way, from the ventricle to the aorta. In Marfan syndrome, as the aorta widens, the aortic valve also is stretched, and the valve flaps cannot close properly. This allows blood to leak the wrong way, from the aorta back into the left ventricle (regurgitation). As a result, the heart has to work harder to pump blood out to the body. The heart can become overworked, leading to heart failure. People with aortic regurgitation may have shortness of breath and exercise intolerance.
- Aortic dissection. This is a tear that occurs in the weakened layers of the inner wall of the aorta. The tear allows blood to get under the inner layer of the wall. As a result, the aorta tears further. An aortic dissection is a life-threatening emergency. Signs and symptoms of an aortic dissection include abrupt onset of chest pain, which may range from mild to severe. There may be pain in the back or the abdomen, or both. The person may sweat, vomit, faint, and have a weak pulse.
Eyes and Vision
Nearsightedness (myopia) is the most common eye problem in people with Marfan syndrome. It can range from mild to severe. People with Marfan syndrome often have astigmatism (a-STIG-ma-tizm), which causes visual distortion and blurred vision.
.
Dislocation of the lens of the eye (ectopia lentis) is another common complication of Marfan syndrome. It is considered a hallmark of Marfan syndrome because it occurs in very few other conditions. It may affect one or both eyes, and the lens may be higher or lower than normal or shifted off to the side. Vision in the affected eye(s) may be severely affected.
.
Other, less common eye problems in Marfan syndrome include detached retina, cataracts, and glaucoma. A detached retina occurs when there are holes or tears in the inner lining of the eye. A cataract is a clouding of the lens. Glaucoma occurs as a result of high pressure in the eye. People with Marfan syndrome tend to get cataracts and glaucoma at a younger age than people who do not have Marfan syndrome.
Lungs
In Marfan syndrome, the air sacs in the lungs may be larger than normal. This can cause breathing problems. People with Marfan syndrome are at an increased risk of developing emphysema or chronic obstructive pulmonary disease (COPD), a serious lung disease.
.
Sudden collapse of the lung, called spontaneous pneumothorax (noo-mo-THOR-aks) can occur in people with Marfan syndrome. About 1 in every 20 people with Marfan syndrome develops this problem. Collapsed lung can happen after only a slight blow to the chest, or even while at rest without a known cause. Collapsed lung usually causes sudden shortness of breath and requires immediate medical attention.
.
Sleep Apnea
Sleep Apnea is a problem that is often associated in the general population with being overweight or obese. But thin people with Marfan syndrome can also suffer from it. Sleep apnea may be due to looseness of the connective tissue in the airways. More on Sleep Apnea and getting Heart Attacks in Early Morning when you wake up
Skin
Stretch marks on the skin occur in about 2 out of every 3 people with Marfan syndrome. The stretch marks are usually on the lower back, buttocks, shoulders, breasts, thighs, and abdomen. They differ from stretch marks in the general population because, in people with Marfan syndrome, they occur without excessive weight gain or loss. The marks usually appear around the time of puberty, but may occur in childhood. They do not require treatment.
.
What Are the Signs and Symptoms of Raynaud’s Disease?
People with Raynaud’s (primary or secondary) have attacks in response to cold or emotional stress. The attacks can affect the fingers and toes, and rarely the nose, ears, nipples, or lips. The affected body parts will usually have two or more of the following changes:
- Look pale due to lack of blood flow
- Look bluish due to a lack of oxygen
- Feel numb, cold, or painful
- Redden and throb or tingle as blood returns to the affected area
Attacks usually last about 15 minutes. They can last less than a minute or as long as several hours. Attacks can occur daily or weekly.
Sometimes attacks affect only one or two fingers or toes. Different areas may be affected at different times. Attacks can cause sores or tissue death (gangrene) in people with severe secondary Raynaud’s. However, severe Raynaud’s is very uncommon.
What Are the Signs and Symptoms of Holes in the Heart?
Atrial Septal Defect
A heart murmur (an extra flow sound associated with the heartbeat) is the most common sign of an atrial septal defect (ASD). Often, it’s the only sign. However, not all murmurs are a sign of a congenital heart defect. Many healthy children have heart murmurs, which are innocent, normal sounds of blood flow through the heart. A doctor can tell by listening whether a murmur is a normal flow sound or a sign of a heart problem. Many babies born with ASDs have no signs or symptoms.
If a large ASD isn’t repaired, the extra blood flow to the right side of the heart can eventually damage the heart and lungs, causing heart failure. This doesn’t occur until adulthood.
Signs and symptoms of heart failure can include:
- Fatigue or tiring easily during exercise or activity
- Shortness of breath
- A buildup of blood and fluid in the lungs
- A buildup of fluid in the feet, ankles, and legs
Ventricular Septal Defect
A heart murmur is usually present in ventricular septal defect (VSD) and may be the first and only sign of this defect. The heart murmur is often present right after birth in many infants, but it may not be heard until the baby is 6 to 8 weeks old.
Most newborns who have VSDs don’t have heart-related symptoms. However, a baby with a medium or large VSD can develop heart failure. Signs and symptoms of heart failure usually appear during the baby’s first 2 months of life. The signs and symptoms of heart failure from VSD are similar to those listed above for ASD, but they occur in infancy.
The major sign of heart failure is difficulty feeding and poor growth. VSD symptoms are rare after infancy because the defect either decreases in size on its own or is repaired.
.
What Are the Signs and Symptoms of Congenital Heart Defects?
Many congenital heart defects have few or no symptoms. A doctor may not even detect signs of a heart defect during a physical exam.
Some heart defects do have symptoms. These depend on the number and type of defects and how severe the defects are. Severe defects can cause symptoms, usually in newborn babies. These symptoms can include:
- Rapid breathing
- Cyanosis (a bluish tint to the skin, lips, and fingernails)
- Fatigue (tiredness)
- Poor blood circulation
Congenital heart defects don’t cause chest pain or other painful symptoms.
Abnormal blood flow through the heart caused by a heart defect will make a certain sound. Your doctor can hear this sound, called a heart murmur, with a stethoscope. However, not all murmurs are a sign of a congenital heart defect. Many healthy children have heart murmurs.
Normal growth and development depend on a normal workload for the heart and normal flow of oxygen-rich blood to all parts of the body. Babies with congenital heart defects may have cyanosis or tire easily when feeding. Sometimes they have both problems. As a result, they may not gain weight or grow as they should.
Older children may get tired easily or short of breath during exercise or activity. Many types of congenital heart defects cause the heart to work harder than it should. In severe defects, this can lead to heart failure, a condition in which the heart can’t pump blood strongly throughout the body.
.
Symptoms of heart failure include:
- Fatigue with exercise
- Shortness of breath
- A buildup of blood and fluid in the lungs
- A buildup of fluid in the feet, ankles, and legs
What Are the Signs and Symptoms of Patent Ductus Arteriosus?
A heart murmur may be the only sign that a baby has patent ductus arteriosus (PDA). A heart murmur is an extra or unusual sound heard during the heartbeat.
Some infants may develop signs or symptoms of volume overload on the heart and excess blood flow in the lungs.
Signs and symptoms may include:
- Fast breathing, working hard to breathe, or shortness of breath, or in the case of a premature infant, need for increased oxygen or ventilatory support
- Poor feeding and poor weight gain
- Tiring easily
- Sweating with exertion (such as while feeding)
What Are the Signs and Symptoms of Tetralogy of Fallot?
An important symptom of tetralogy of Fallot is cyanosis, or a bluish tint to the skin, lips, and fingernails. Low levels of blood in the oxygen cause this symptom.
Babies with tetralogy of Fallot sometimes have “tet spells” in response to an activity like crying or having a bowel movement. A “tet spell” occurs when the oxygen level in the blood suddenly drops. This causes the baby to become very blue. The baby may also:
- Have a hard time breathing
- Become very tired and limp
- Not respond to a parent’s voice or touch
- Become very fussy
- Lose consciousness
In years past, when tetralogy of Fallot wasn’t treated in infancy, children would get very tired during exercise and could have fainting spells. This heart defect is now repaired in infancy to prevent symptoms like this.
.
Another common symptom of tetralogy of Fallot is a heart murmur. A heart murmur is an extra or unusual sound that a doctor can hear while listening to the heart during a physical exam. When a heart defect causes an abnormal flow of blood through the heart, it will make a certain sound. However, not all murmurs are signs of congenital heart defects. Many healthy children have heart murmurs.
Normal growth and development depend on a normal workload for the heart and normal flow of oxygen-rich blood to all parts of the body. Babies who have tetralogy of Fallot may not gain weight or grow as quickly as children with healthy hearts because they tire easily while feeding.
.
Children with this heart defect also may have “clubbing,” an abnormal, rounded shape to the skin or bone around the fingernails.
What Are the Signs and Symptoms of Holes in the Heart?
Atrial Septal Defect
A heart murmur (an extra flow sound associated with the heartbeat) is the most common sign of an atrial septal defect (ASD). Often, it’s the only sign. However, not all murmurs are a sign of a congenital heart defect. Many healthy children have heart murmurs, which are innocent, normal sounds of blood flow through the heart. A doctor can tell by listening whether a murmur is a normal flow sound or a sign of a heart problem. Many babies born with ASDs have no signs or symptoms.
If a large ASD isn’t repaired, the extra blood flow to the right side of the heart can eventually damage the heart and lungs, causing heart failure. This doesn’t occur until adulthood.
Signs and symptoms of heart failure can include:
- Fatigue or tiring easily during exercise or activity
- Shortness of breath
- A buildup of blood and fluid in the lungs
- A buildup of fluid in the feet, ankles, and legs
Ventricular Septal Defect
A heart murmur is usually present in ventricular septal defect (VSD) and may be the first and only sign of this defect. The heart murmur is often present right after birth in many infants, but it may not be heard until the baby is 6 to 8 weeks old.
Most newborns who have VSDs don’t have heart-related symptoms. However, a baby with a medium or large VSD can develop heart failure. Signs and symptoms of heart failure usually appear during the baby’s first 2 months of life.
The signs and symptoms of heart failure from VSD are similar to those listed above for ASD, but they occur in infancy.
The major sign of heart failure is difficulty feeding and poor growth. VSD symptoms are rare after infancy because the defect either decreases in size on its own or is repaired.
What Are the Signs and Symptoms of Peripheral Arterial Disease?
At least half of the people who have peripheral arterial disease (PAD) don’t have any signs or symptoms of the disease.
People who do have signs or symptoms may have pain when walking or climbing stairs, which may be relieved after resting. This pain is called intermittent claudication (klaw-de-KA-shen). Blood brings oxygen to the muscles, but during exercise, muscles need more blood flow. If there is a blockage in the blood vessels, muscles won’t get enough blood. If a person has intermittent claudication and exercises while in pain, his or her muscles may be harmed. When resting, the muscles require less blood flow and the pain goes away. Claudication is more likely in people who also have atherosclerosis in other arteries, such as the heart and brain. About 10 percent of people with PAD have intermittent claudication.
.
Other signs and symptoms of PAD include:
- Pain, numbness, aching, and heaviness in the muscles
- Cramping in the legs, thighs, calves, and feet
- A weak or absent pulse in the legs or feet
- Sores or wounds on toes, feet, or legs that heal slowly, poorly, or not at all
- Color changes in skin, paleness, or blueness (called cyanosis)
- A decreased temperature in one leg compared to the other leg
- Poor nail growth and decreased hair growth on toes and legs
- Erectile dysfunction, especially among people with diabetes
.
Source: National Heart, Lung, Blood Institute of US Dept of Health & Human Services
http://www.nhlbi.nih.gov
.
10 Year Heart Attack Risk Calculator:
Calculate your risk of heart attack with this simple Heart Attack Risk Calculator at:
http://hp2010.nhlbihin.net/atpiii/calculator.asp?usertype=pub
teamrich.wordpress.com – heart attack signs
.
 In 2006, 22 of the chemicals that are in most haircolor products including PPD were banned in Europe. These “hair care” products are not regulated by FDA in the USA so claims of its safety are also not regulated either. In 2008, the WHO (World Health Organisation) said that there is evidence that hair dyes can increase the risk of bladder cancer for male hairstylists and hair colorists.
In 2006, 22 of the chemicals that are in most haircolor products including PPD were banned in Europe. These “hair care” products are not regulated by FDA in the USA so claims of its safety are also not regulated either. In 2008, the WHO (World Health Organisation) said that there is evidence that hair dyes can increase the risk of bladder cancer for male hairstylists and hair colorists. Henna is a plant that is also used for ayurvedic hair coloring. Henna should not be used on gray hair, as it turns it orange. Henna is derived from the leaves of the shrub Lawsonia inermis, which grows in India, North Africa and Sri Lanka; lawsone is the active dye ingredient. The major disadvantage of henna is it cannot be used to lighten one’s natural hair color.
Henna is a plant that is also used for ayurvedic hair coloring. Henna should not be used on gray hair, as it turns it orange. Henna is derived from the leaves of the shrub Lawsonia inermis, which grows in India, North Africa and Sri Lanka; lawsone is the active dye ingredient. The major disadvantage of henna is it cannot be used to lighten one’s natural hair color.